Some big changes are happening with our company.
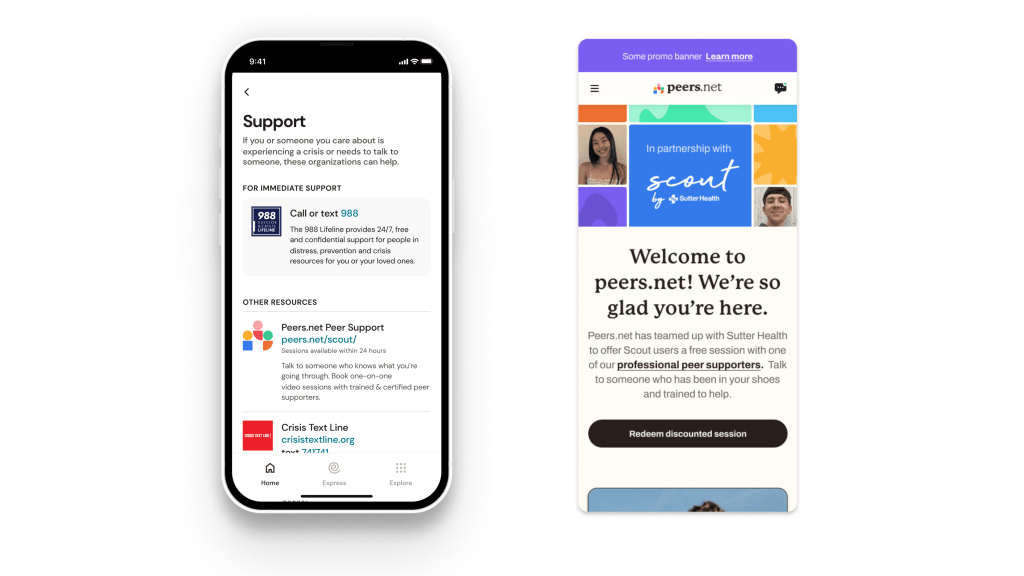
Earlier this year we made the tough decision that our Peers.net peer support service would grow faster and have more impact within a larger organization. Peers.net is moving to WellSpace Health, a nonprofit community health system which provides medical and mental health care to over 130,000 Medicaid and uninsured patients and runs the 988 crisis line in Northern California.
Our head of peer support, Jammie Gardner, and our care coordinator, Rebecca Young, are joining WellSpace, along with our California-based peers. Peers.net service is currently suspended while they are going through onboarding at WellSpace, but will resume soon. WellSpace is also continuing our accredited training program, using our scalable online model to train more young adults as peer support specialists and community health workers.
Kim Newell Green, MD FAAP and I co-founded Flourish Labs just after the pandemic to scale peer support as a solution to the youth mental health crisis. Our founding story was personal as well as data-driven. We saw the shortage of mental health professionals in our home and work lives, and had personally experienced the power of peer support through family members struggling with addiction. Peer support is evidence-based but underutilized: many people don’t know about it as an alternative to therapy, it’s rarely available via telehealth, and insurance coverage is limited.
We built Peers.net to change that, with a team of healthcare, peer support and tech experts. We co-created with young adults and teens to launch a mental health service optimized for Gen Z, giving them a choice of providers by shared lived experience and identity (we’re proud that half of our peers identify as LGBTQ+ and BIPOC). We demonstrated that Medicaid and commercial health plans will reimburse peer support, signing contracts in 5 states covering 10 million lives. We trained over 100 young adults as peer support specialists, and could have trained thousands – we received over 4,000 job applications. We delivered high-quality service to nearly 1000 young people, with 95% saying they were extremely satisfied and 93% saying they had an excellent therapeutic alliance with their peer. We received incredible testimonials about the profound impact of feeling truly seen and heard. We profoundly changed lives, and in some cases saved the lives of those we reached.
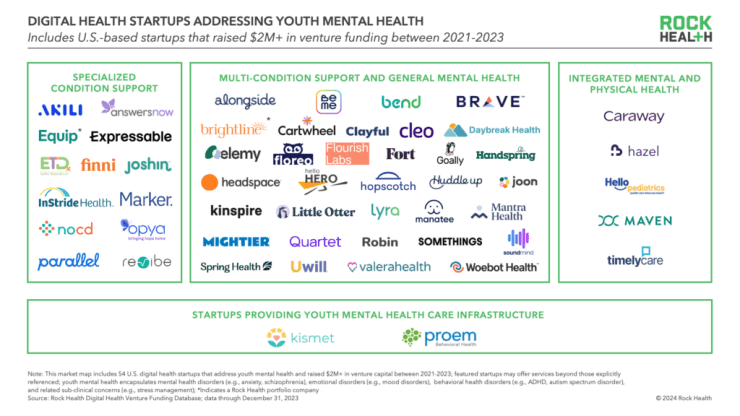
However, we didn’t scale to our impact and revenue goals. Everyone knows there’s massive demand for youth mental health services: 34% of teens and young adults struggle with mental illness, and over half get no care. Despite this, finding clients and enrolling them into our service proved challenging. We’re not alone in this struggle. Many digital health companies we spoke to face similar patient acquisition challenges as search is disrupted by LLMs, ads are becoming ever more expensive, and activating provider referral channels takes enormous effort and time.
Earlier this year we made the tough decision that Peers.net would grow faster and have more impact within a larger organization. WellSpace Health shares our commitment to peer support and already includes peers in their clinic-based care model. Our telehealth and AI technology will help them expand their tech capabilities and geographical reach.
The bittersweet part: Since WellSpace is focused on California, we’ve ended our operations and health plan contracts in Oregon, Nevada, Washington DC and New Jersey. Many of our team won’t be moving to WellSpace, including Kim and myself. Some of our team already have new roles, others are looking for their next opportunities.
💃 You’d be lucky to have Erika Rowen, Hannah Schilpp, Paola Veglio and Kim Newell Green, MD FAAP on your team. Our talented peer supporters Rilynn McClain-Small, Arianna J., Eli Mendoza, Layla Ghazalba, Gertrude Nakibuule, Julia Parker, Alexzander Chross, Jonathan Mortenson, Myra Kelly, Nina Smith are also seeking new roles. Please DM me if you can help them.
🙏 Thank you
We’re deeply grateful that our mission – scaling peer support through telehealth and AI to address the youth mental health crisis – will continue and grow. We built something meaningful that will outlast our company. Thank you to the WellSpace team A. Jonathan Porteus, PhD, Christie Gonzales, Dr. Janine Bera, Cordia Losh and Ben Renteria for taking on the baton to grow peer support for young people.
A big big thank you to everyone who believed in our vision and joined our journey, especially our incredible team, investors, advisors, and partners made this work possible. We learnt from so many incredible people how to build Peers.net, including teens and young adults, peers, mental health industry experts, and other founders.
to our team:

Kim Newell Green, MD FAAP, Adrian Koren, Alex Weisman, Ally Linfoot, Claire Bradley, Erika Rowen, Hannah Schilpp, Jammie Gardner, Julia Tasiopoulos, Paola Veglio and Rebecca Young
to our investors:
Anna Patterson and Andrew Brackin at Gradient
Luisa Sucre, Craig Dalton, Guy Vidra and Craig Shapiro at Collaborative Fund
Carmine Di Maro and Pushkar Joshi, PhD at the One Mind accelerator
Jason Lehmbeck , Lisa Hepburn and Matthew Biel at the Georgetown University Thrive accelerator
Carrie Walton Penner , John Bailey and Judy Park at Fiore Ventures LLC
Don Burton and Rob Hutter at Learn Capital
Philipp Moehring and Andy Chung at Tiny Supercomputer Investment Company
Peggy Cheng and Brian Li at Authentic Heart Foundation
Santi Dewa Ayu and David Ball at the Headstream Innovation accelerator
to our angels (many founders who gave us the best advice!)
Christina Wire & Jeremy Wire
Helen Riley & Jean-Philippe Emelie Marcos
Iyah Romm & Sylvia Romm, MD, MPH
John Mayerhofer & Nina Mayerhofer
Margo Georgiadis and Pantelis A. “Pete” Georgiadis
Raffi Grinberg & Charlotte Grinberg
to our advisors & partners:
Alison Malmon at Active Minds, Inc.
Amanda Galton at Orrick, Herrington & Sutcliffe LLP
Dana Foglesong and Lisa Mariani at Magellan Health
Darshan Gupta and Urvik Patel at Infocusp Innovations
Greg Hajcak at Santa Clara University
Jacinda Shelly at Apero Health (Y Combinator)
Karen Black at Carelon Behavioral Health
Kelly Davis at Mental Health America
Keanan Joyner at University of California, Berkeley
Manpreet Kaur Singh at University of California, Davis
Marc Goldsand at Goldsand Friedberg
Rachel Kotok Goldberg at NovaWell Horizon
Samuel McLean at University of North Carolina at Chapel Hill
Samantha Baker at PacificSource Health Plans
to our peer advisory board:
Wow that’s a long list! It takes a village, as Kim always says.
With love & gratitude,
Obi